Products Category
- FM Transmitter
- 0-50w 50w-1000w 2kw-10kw 10kw+
- TV Transmitter
- 0-50w 50-1kw 2kw-10kw
- FM Antenna
- TV Antenna
- Antenna Accessory
- Cable Connector Power Splitter Dummy Load
- RF Transistor
- Power Supply
- Audio Equipments
- DTV Front End Equipment
- Link System
- STL system Microwave Link system
- FM Radio
- Power Meter
- Other Products
- Special for Coronavirus
Products Tags
Fmuser Sites
- es.fmuser.net
- it.fmuser.net
- fr.fmuser.net
- de.fmuser.net
- af.fmuser.net ->Afrikaans
- sq.fmuser.net ->Albanian
- ar.fmuser.net ->Arabic
- hy.fmuser.net ->Armenian
- az.fmuser.net ->Azerbaijani
- eu.fmuser.net ->Basque
- be.fmuser.net ->Belarusian
- bg.fmuser.net ->Bulgarian
- ca.fmuser.net ->Catalan
- zh-CN.fmuser.net ->Chinese (Simplified)
- zh-TW.fmuser.net ->Chinese (Traditional)
- hr.fmuser.net ->Croatian
- cs.fmuser.net ->Czech
- da.fmuser.net ->Danish
- nl.fmuser.net ->Dutch
- et.fmuser.net ->Estonian
- tl.fmuser.net ->Filipino
- fi.fmuser.net ->Finnish
- fr.fmuser.net ->French
- gl.fmuser.net ->Galician
- ka.fmuser.net ->Georgian
- de.fmuser.net ->German
- el.fmuser.net ->Greek
- ht.fmuser.net ->Haitian Creole
- iw.fmuser.net ->Hebrew
- hi.fmuser.net ->Hindi
- hu.fmuser.net ->Hungarian
- is.fmuser.net ->Icelandic
- id.fmuser.net ->Indonesian
- ga.fmuser.net ->Irish
- it.fmuser.net ->Italian
- ja.fmuser.net ->Japanese
- ko.fmuser.net ->Korean
- lv.fmuser.net ->Latvian
- lt.fmuser.net ->Lithuanian
- mk.fmuser.net ->Macedonian
- ms.fmuser.net ->Malay
- mt.fmuser.net ->Maltese
- no.fmuser.net ->Norwegian
- fa.fmuser.net ->Persian
- pl.fmuser.net ->Polish
- pt.fmuser.net ->Portuguese
- ro.fmuser.net ->Romanian
- ru.fmuser.net ->Russian
- sr.fmuser.net ->Serbian
- sk.fmuser.net ->Slovak
- sl.fmuser.net ->Slovenian
- es.fmuser.net ->Spanish
- sw.fmuser.net ->Swahili
- sv.fmuser.net ->Swedish
- th.fmuser.net ->Thai
- tr.fmuser.net ->Turkish
- uk.fmuser.net ->Ukrainian
- ur.fmuser.net ->Urdu
- vi.fmuser.net ->Vietnamese
- cy.fmuser.net ->Welsh
- yi.fmuser.net ->Yiddish
COVID-19 Vaccination: 10 Key Things You Need To Know About

What does the COVID-19 vaccine have to do with me? Is the COVID-19 vaccination safe? The following article will give you a detailed introduction to all the information you need to know about the COVID-19 vaccine. Let’s take a look.
---- WEAR MASK AND STAY SAFE ----
1. Why COVID-19 Vaccination Is Important to ME?
2. How Many Types of Legal COVID-19 Vaccines Are There For the Vaccination?
3. What Are the Current COVID-19 Vaccine Manufacturers I Can Trust?
4. How Do These Types of Coronavirus Vaccine Approaches Work?
5. Here Are the Authorized and Recommended Vaccines For YOU
6. 10 Secrets They Will Not Tell You About The COVID-19 Vaccination
7. What is the Souce of the COVID-19 Pandemic?
8. Facts You Should Know About The COVID-19
9. What's The Difference Flu Virus and COVID-19 Virus?
10. 10 Best Ways To Protect You And Others From The COVID-19
Why COVID-19 Vaccination Is Important to ME?
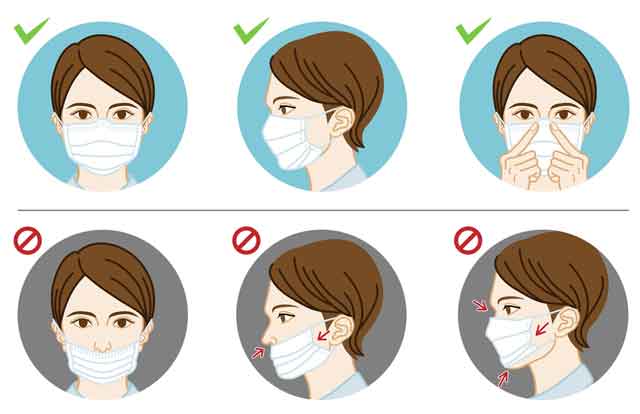
Since the outbreak of COVID-19, there have been countless economic losses and casualties. And due to the sudden outbreak of COVID-19 and its high infectivity, governments in various countries did not have good control methods and effective methods to prevent their people from getting infected by the coronavirus in the early stage of the spread of COVID-19. (Most common and effective measure to prevent you from the COVID-19 virus is to wear a mask, and the most effective way to fight against the COVID-19 is the COVID-19 vaccination)
Source: UT Southwestern
We list the major Top 20 large-number cases countries of infected cases, the deceased, the recovered. According to the latest report from Johns Hopkins University, the cumulative cases around the world has come up to 81,294,343. While the global death has come up to 1,77439,5 and 9,807,569 for the cured.
|
Infected Cases Countries Top 20 |
Recovered Cases Top 20 |
Death Cases Top 20 |
|
25,437,225 US
10,676,838 India
8,933,356 Brazil
3,716,228 Russia
3,700,268 United Kingdom
3,138,498 France
2,629,817 Spain
2,485,956 Italy
2,442,350 Turkey
2,164,043 Germany
2,041,352 Colombia
1,885,210 Argentina
1,771,740 Mexico
1,482,722 Poland
1,423,578 South Africa
1,385,706 Iran
1,237,810 Ukraine
1,102,795 Peru
1,012,350 Indonesia
970,156 Netherlands
|
425,062 US
218,878 Brazil
153,587 India
150,273 Mexico
100,359 United Kingdom
86,422 Italy
74,250 France
69,391 Russia
57,560 Iran
56,794 Spain
53,619 Germany
52,128 Colombia
47,253 Argentina
41,797 South Africa
39,887 Peru
35,665 Poland
28,468 Indonesia
25,344 Turkey
23,148 Ukraine
Belgium 20,814
|
10,345,985 India
7,896,290 Brazil
3,140,930 Russia
2,322,511 Turkey
1,917,117 Italy
1,864,904 Colombia
1,863,959 Germany
1,674,555 Argentina
1,335,876 Mexico
1,254,674 South Africa
1,243,575 Poland
1,177,367 Iran
1,012,450 Peru
999,466 Ukraine
831,394 Czechia
820,356 Indonesia
684,817 Canada
662,460 Chile
658,595 Romania
584,752 Iraq
|
| TOTAL: 100,221,840 | TOTAL: 2,155,052 | TOTAL: 55,329,184 |
|
*Last Updated at 27/1/2021 11.26: P.M. *Data Sources: Johns Hopkins University (JHU) - More
|
||
At present, these numbers are still expanding, which means that the impact of the COVID-19 virus is also expanding, but the good news is that the legally injectable COVID-19 vaccine on the market has been developed and put into use, please Don't worry too much.
However, FMUSER would like to remind you that when you go out, please wear a mask and take disinfection measures to prevent infection by the COVID-19 virus. If you find any abnormal symptoms, please seek medical attention in time.
Many people worry that as the impact of the COVID-19 epidemic continues to expand, it will not only affect your current daily life but also your daily life in the future. When you wear a mask and take disinfection measures and think that everything is ALL RIGHT, but people around you are constantly infected by the COVID-19 virus, that's NOT ALL RIGHT!
I wonder if you are thinking of a better solution to prevent being affected by the COVID-19 virus, especially when you have a family, this need is even more urgent.
However, please don’t worry, FMUSER will give you a detailed introduction to all the solutions you need to prevent COVID-19 virus infection. Let’s start with introducing the COVID-19 vaccine!
How Many Types of Legal COVID-19 Vaccines Are There For the Vaccination?
● Types of the COVID-19 Vaccine from Different Groups
As the Pfizer-BioNTech COVID-19 vaccine is being evaluated by the U.S. Food and Drug Administration (FDA) and the Moderna vaccine is soon to follow, according to the research of FMUSER, we found out that there are 4 main types of legal COVID-19 vaccine for the vaccination ( NOTE: The U.S. government has already acquired millions of doses from domestic and European companies and pledged to offer them free to the U.S. population, although healthcare facilities may charge for administering the doses) and they are:
 |
 |
 |
 |
|
mRNA VACCINE |
VECTOR VACCINES |
PROTEIN SUBUNIT VACCINE |
WHOLE, KILLED VACCINES |
|
Used by: Pfizer, Moderna |
Used by: AstraZeneca, Janssen, Sputnik
|
Used by: Novavax, Sanofi |
Used by: Sinovac |
|
Doses: 2 |
Doses: 1- 2 |
Doses: 1 - 2 |
Doses: 1 - 2 |
|
mRNA vaccines are the newest approach. They use genetic material called messenger RNA, a kind of genetic software that instructs cells to make a piece of the coronavirus spike protein. That will get the attention of the immune system. The mRNA is coated in soft fatty lipids to protect it. |
Vector vaccines use another virus to carry in the genetic instructions to make the spike protein. For coronavirus they all use adenoviruses, a type of common cold virus. They attach to cells and inject DNA that tells the cells to make coronavirus spike protein. |
Vector vaccines use another virus to carry in the genetic instructions to make the spike protein. For coronavirus they all use adenoviruses, a type of common cold virus. They attach to cells and inject DNA that tells the cells to make coronavirus spike protein. |
Protein subunit vaccines just get little pieces of the target virus circulating in the system for the immune system to find and recognize. Instead of using the human body as the vaccine factory, genetically engineered insect viruses are used to infect moths, whose cells then produce the pieces of coronavirus spike protein. These are harvested and made into a vaccine |
What? DON'T KNOW what I'm saying? Let's take a quick review on the "The 4 Types of COVID-19 Vaccines"
What Are the Current COVID-19 Vaccine Manufacturers I Can Trust?
Well, based on the information researched by FMUSER above, you should have a certain understanding of the role of the current COVID-19 vaccine and the working principle of the COVID-19 vaccine, but you may still ask, since there are so many COVID-19 vaccines , But which COVID-19 vaccine manufacturer is the most trustworthy? FMUSER can't immediately decide for you which COVID-19 vaccine is most suitable for you, but FMUSER can provide you with first-hand information on COVID-19 manufacturers. Let's take a look at their background stories and corporate strength!

● 6 Trustworthy Groups Producers of The COVID-19 Vaccine
On November 16, Moderna issued a preliminary data readout out of its COVID-19 vaccine, suggesting an efficacy rate of 94.5%. Like the Pfizer-BioNTech vaccine, it is an mRNA vaccine. Unlike that vaccine, however, the Moderna vaccine is stable at 36 to 46 degrees F, about the temperature of a standard home or medical refrigerator, for up to 30 days and can be stored for up to six months at -4 degrees F. It is expected to go to the FDA for consideration for a EUA within days.
On November 23, AstraZeneca and the University of Oxford announced high-level results from an interim analysis of their COVID-19 vaccine, AZD1222. The analysis was from the trials in the UK and Brazil and demonstrated the efficacy of up to 90%. The vaccine was effective at preventing COVID-19, with no hospitalizations or severe cases in people receiving it. There were a total of 131 COVID-19 positive cases in the interim analysis group. One dosing regimen was given at a half dose and demonstrated 90% efficacy, followed by a full dose at least one month apart. Another dosing regimen demonstrated 62% efficacy when given two full doses at least one month apart. The combined analysis showed average efficacy of 70%. The AstraZeneca vaccine can be stored, transported, and handled at normal refrigerated conditions, about 36-46 degrees F, for at least six months and administered within existing healthcare settings.
Johnson & Johnson
Johnson & Johnson announced on November 15 that it initiated a second global Phase III trial of its Janssen COVID-19 vaccine. They expect to enroll up to 60,000 volunteers worldwide.
Whereas all of the other three vaccine candidates require two doses about 28 days apart, the J&J vaccine only requires a single dose. Interim results from its Phase I/IIa trial demonstrated a single dose of the vaccine-induced a robust immune response and was generally well-tolerated. The ENSEMBLE 2 study evaluated a two-dose regimen as well.
Russia’s Sputnik V Vaccine
Around November 11, Russia’s National Research Center for Epidemiology and Microbiology, which Russia authorized for use in August—ahead of even beginning a Phase III trial—claimed had an efficacy rate of 92% after the second dose. It was based on a first interim analysis 21 days after the first injection during the ongoing Phase III study. On November 24, the organization claimed 95% efficacy based on new preliminary data. It also offered to share one of its two human adenoviral vectors with AstraZeneca to increase the efficacy of the AstraZeneca vaccine.
Russia approves Covid-19 vaccine 'Sputnik V': Why's the world sceptical?
|
Brand Name |
Type |
Doses |
Likely EUA Date |
Doses by Year-End |
Price |
|
Pfizer-BioNTech |
mRNA |
2, 28 Days Apart |
December 10, 2020 |
~50 Million |
$19.50 per dose for the first 100 million doses |
|
Moderna |
mRNA |
2, 28 Days Apart |
December 10, 2020 |
50 Million |
$25-$37 per dose |
|
AstraZeneca-University of Oxford |
Adenovirus-based |
2, 28 Days Apart |
Possibly January 2021, but unclear in the U.S. |
Potentially 30 Million |
$3 per dose, potentially, but variable by market |
|
Johnson & Johnson |
Adenovirus-based |
1 |
Possibly March or April 2021 |
Projects 1 billion by end of 2021 |
$10 per dose |
|
Russia’s Sputnik V Vaccine |
Adenovirus-based |
2 |
Not applicable in the U.S. |
Projects 500 million by end of 2021 |
$10 per dose |
|
Name |
Macrophages |
B-lymphocytes |
T-lymphocytes |
|
Category |
white blood cells |
defensive white blood cells |
defensive white blood cell |
|
Functions |
swallow up and digest germs and dead or dying cells |
produce antibodies that attack the pieces of the virus left behind by the macrophages. |
produce antibodies that attack the pieces of the virus left behind by the macrophages. |
| How it works |
The macrophages leave behind parts of the invading germs called antigens. The body identifies antigens as dangerous and stimulates antibodies to attack them. |
B-cells become "activated" when they encounter foreign antigens, as in foreign markers on the outside of bacteria cells during an infection |
According to the CDC, the main cause of our illness is that bacteria have invaded our body and continued to multiply in our body, attacking our body. At this time, our immune system works. Although different immune system cells are responsible for Different responsibilities, but all serve the same immune system. |
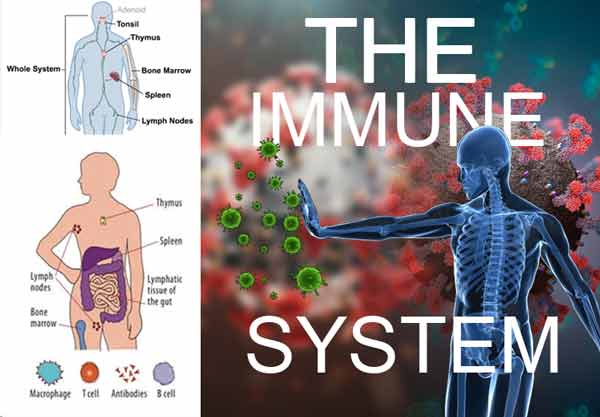
● After vaccination, it takes several weeks for the body to produce T lymphocytes and B lymphocytes
● The vaccine will not take effect immediately, so you may still be infected with the virus within a few weeks after it takes effect
● After vaccination, there will be fever and other symptoms, indicating that immunity is increasing
| Diagram |
 |
 |
 |
 |
 |
|
Types of vaccines |
DNA and RNA |
live-attenuated |
Inactived |
Subunit |
Viral Vector |
|
Advantages |
Easy and quick to design.
|
Stimulates a robust immune response without causing serious disease. |
Safe because the virus is already dead and is easy to make.
|
Focuses the immune response on the most important part of the virus for protection and cannot cause infection. |
Live viruses tend to elicit stronger immune responses than dead viruses or submit vaccines. |
|
Disadvantages
|
Never been done before. There are so licensed DNA or RNA vaccines currently in use. |
May not be safe for those wit compromised immune systems. |
Not as effective as a live virus. Some previous inactived vaccines have made the disease worse; safety for thenovel coronavirus needs to be shown in clinical trials. |
May not stimulate a strong response, other chemiclas may need to be added to boost long-term immunity. |
Important to pick a viral vector thatis truly safe. An immune reponse to the viral vector could make the vaccine less effective. |
|
How it works |
This vaccine uses DNA and RNA moleclues to teach the immune system to target key viralproteins. |
This is a weakened version of the actual virus. |
An inactivated vaccine uses the whole virus after it has been killed with heat or chemicals. |
This vaccine uses a piece of a virus' surface to focus your immune system on a single target. |
This approach takes a harmless virus and uses it to deliver viral genes to buld immunity. |
| Existing examples |
● None |
● Measles, Mumps and Rubella ● Chickenpox |
● Polio |
● Pertussis ● Hepatitis B ● Human papillomavirus |
● Ebola ● Veterinary medicine |
|
Group testing this approach for COVID-19 |
● Moderna (RNA) ● Inovio (DNA) |
● Codagenix ● Indian Immunologicals Ltd. |
● Sinovac ● Sinopharm |
● Novavax ● AdaptVac |
● University of Oxford & AstraZeneca ● CanSino Biologics ● Johnson & Johnson |
As COVID-19 vaccines are authorized and then recommended for use in the United States, it will be important to understand what is known about each vaccine. FMUSER will provide information on who is and is not recommended to receive each vaccine and what to expect after vaccination, as well as ingredients, safety, and effectiveness.
Currently, two vaccines are authorized and recommended to prevent COVID-19:
● Moderna’s COVID-19 vaccine
● Vaccines in Phase 3 Clinical Trials
● AstraZeneca’s COVID-19 vaccine
● Janssen’s COVID-19 vaccine
● Novavax’s COVID-19 vaccine
10 Secrets They Will Not Tell You About The COVID-19 Vaccination
A1: NO, IT WON'T.
The COVID-19 vaccines will not give you COVID-19. On the contrary, COVID-19 vaccination will be a much safer way to protect you from the COVID-19. Sometimes this process can cause symptoms, such as fever. These symptoms are normal and are a sign that the body is building immunity.
A2: NO, IT WON'T.
Neither the recently authorized and recommended vaccines nor the other COVID-19 vaccines currently in clinical trials in the United States cause you to test positive on viral tests, which are used to see if you have a current infection.
If your body develops an immune response, which is the goal of vaccination, there is a possibility you may test positive on some antibody tests. Antibody tests indicate you had a previous infection and that you may have some level of protection against the virus. Experts are currently looking at how COVID-19 vaccination may affect antibody testing results.
A3: Currently NO
Due to the severe health risks associated with COVID-19 and the fact that re-infection with COVID-19 is possible, people may be advised to get a COVID-19 vaccine even if they have been sick with COVID-19 before.
At this time, experts do not know how long someone is protected from getting sick again after recovering from COVID-19. The immunity someone gains from having an infection, called natural immunity, varies from person to person. Some early evidence suggests natural immunity may not last very long.
No one knows how long immunity produced by vaccination lasts until we have more enough data on how well it works.
A4: NO, IT WON'T.
COVID-19 vaccination can help prevent getting sick with COVID-19. While many people with COVID-19 have only a mild illness, others may get a severe illness or they may even die. There is no way to know how COVID-19 will affect you, even if you are not at increased risk of severe complications. If you get sick, you also may spread the disease to friends, family, and others around you while you are sick. COVID-19 vaccination helps protect you by creating an antibody response without having to experience sickness.
A5: NO. IT WON'T
mRNA stands for messenger ribonucleic acid and can most easily be described as instructions for how to make a protein or even just a piece of a protein. mRNA is not able to alter or modify a person's genetic makeup (DNA). The mRNA from a COVID -19 vaccine never enter the nucleus of the cell, which is where our DNA are kept. This means the mRNA does not affect or interact with our DNA in any way. Instead, COVID-19 vaccines that use mRNA work with the body's natural defenses to safely develop protection (immunity) to disease. Learn more about how COVID-19 mRNA vaccines work.
A6: Currently NO.
There are currently no available vaccines that will prevent COVID-19.
It is worth mentioning that flu vaccination can prevent you from catching flu at the same time as COVID-19, but it will not protect you from COVID-19. FMUSER hereby suggests that the most effective way to isolate COVID-19 is not to go to less crowded places, wear masks and do all disinfection work, remember to ventilate and drink more water.
A7: YES, IT IS.
The use of masks and other protective equipment or other protective methods can help reduce the impact of droplet transmission and reduce the risk of disease. However, vaccination is as important as these protective measures. Vaccination can effectively improve the body’s immune system and avoid Your body is violated by the COVID-19 virus, so vaccinations are necessary.
A8: Currently NO
In fact, none of the parties involved in the study of the COVID-19 virus has no effective evidence that taking any specific drug will cause COVID-19 to cause more serious illness. However, if you are vaccinated and taking certain drugs that cause any serious symptoms, please wear your mask, ask your nearest hospital for help and report your condition to your doctor.
It is worth noting that
• Any changes to medications should be made after talking with a healthcare provider.• If you have any questions or concerns, please contact your healthcare provider.
A9: NO, THERE ARE.
Scientists began Phase 1 trials of an experimental vaccine for COVID-19 in mid-March. The vaccine, called mRNA-1273, is being co-developed by researchers at NIH's National Institute of Allergy and Infectious Diseases (NIAID) and the biotech company Moderna, Inc.-More
A10: Currently NO.
The main challenge in developing vaccines against emerging infectious diseases is that each pathogen uses different mechanisms to infect cells and cause different immune responses in the human body. In addition, the cost of developing a new crown vaccine is relatively high, so the produing amount is small, and currently it can’t meet everyone’s needs
The recent emergence of the novel coronavirus behind the COVID-19 pandemic has thrown a spotlight on the risks that animals can pose to humans as the source of new viruses. The virus in question, known as SARS-CoV-2, had never been seen before, so it quickly gained the attention of scientists around the world.
Epidemiologists did field investigations to find out how the new virus started. They conducted surveys in the community and in health facilities and collected nose and throat specimens for lab analyses. These investigations showed them who was infected, when they became sick, and where they had been just before they got sick.
The COVID-19 has been linked to a "wet market" for wild animal trade in Wuhan, China, although it's by no means certain this was the source of the human version of the virus. Bats have been identified as the animal with the closest known equivalent virus although, again, we're not sure that a bat provided the direct origin of SARS-CoV-2.
Using this information, epidemiologists determined that the virus possibly came from an animal sold at a market. The new virus was found to be a coronavirus, and coronaviruses cause the severe acute respiratory syndrome. This new coronavirus is similar to SARS-CoV, so it was named SARS-CoV-2 The disease caused by the virus was named COVID-19 (COronVIrusDisease-2019) to show that it was discovered in 2019.
An outbreak is called an epidemic when there is a sudden increase in cases. As COVID-19 began spreading in Wuhan, China, it became an epidemic. Because the disease then spread across several countries and affected a large number of people, it was classified as a pandemic.
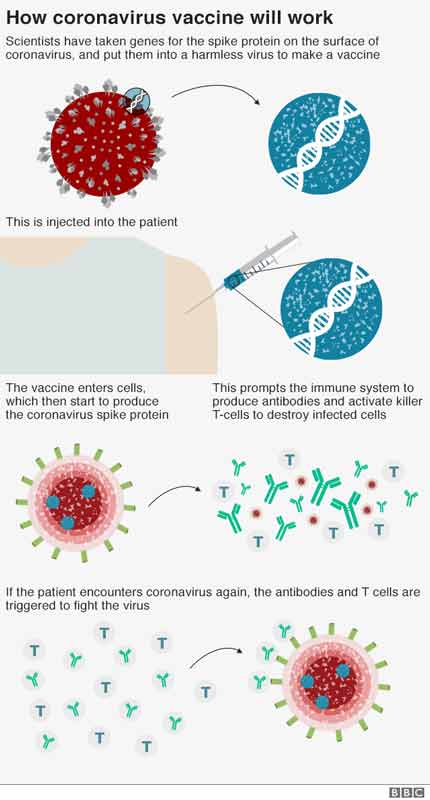
# How Coronavirus Will Work #
Source: BBC
| NOTE: Please keep in mind that although COVID-19 is a disease caused by a coronavirus, not every coronavirus causes COVID-19. | |
|
Official Name |
SARS-CoV-2 |
|
Belongs to |
Ortho Coronaviridae |
|
Affection |
Cause Coronavirus Disease |
|
May Cause |
SARS - Severe Acute Respiratory Syndrome
MERS - Middle East Respiratory Syndrome
COVID-19 - 2019 Novel (New) Coronavirus
Flu - Influenza
|
|
Virus vector |
Human Being |
|
Propagation mode |
From Person to Person |
|
Outbreak Time Limit |
2-14 Days |
|
Infection manifestations |
Mild Symptoms to Severe Illness |
|
PEOPLE WHO MIGHT GET SEVERE SYMPTOMS |
● Older Adults The greatest risk for severe illness from COVID-19 is among those aged 85 or older.● People with Certain Medical Conditions They are at increased risk for severe illness from the virus that might cause COVID-19 ● Other People Who Need Extra Precaution Information for other populations like rural communities, people experiencing homelessness, and people with disabilities.
|
|
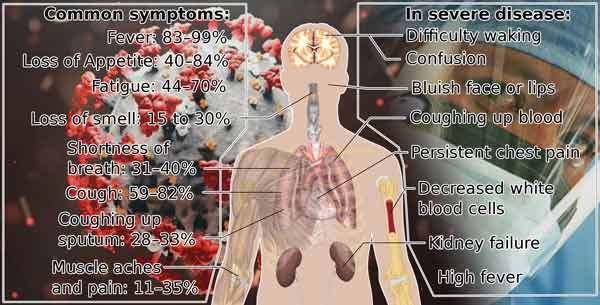
SYMPTOMS MIGHT BE INFECTED BY THE COVID-19 |
● Fever or chills ● Cough● Shortness of breath or difficulty breathing ● Fatigue ● Muscle or body aches ● Headache ● New loss of taste or smell ● Sore throat ● Congestion or runny nose ● Nausea or vomiting ● Diarrhea
|
|
PROTECT YOURSELF BY TAKING THESE STEPS |
● Avoid close contact with people who are sick ● Wash your hands frequently, using soap and running water each time, for at least 20 seconds. If there is no water, please use a hand sanitizer with at least 60% alcohol content instead● Develop good breathing hygiene habits, cover coughing and sneezing with paper towels, and discard the used paper towels in time to keep your hands clean ● Always wash your hands before touching your eyes, nose and mouth ● Develop a good habit of washing your hands every time you go home. Please provide disposable hand sanitizer when someone visits, or please wash your hands immediately after entering the door |
---- This list does not include all possible symptoms. FMUSER will continue to update this list as we learn more about COVID-19. ----
What's The Difference Flu Virus and COVID-19 Virus?
Because some symptoms of influenza and COVID-19 are similar, it may be difficult to distinguish the difference between them based on symptoms alone, and tests may be required to help confirm the diagnosis. Influenza and COVID-19 have many characteristics, but there are some key differences between the two.
|
Signs and Symptoms |
Influenza |
COVID-19(at least two of the following) |
|
Symptom onset |
Sudden |
Gradual |
|
Chills |
Common |
Common |
|
Headache |
Prominent |
Common |
|
Cough |
Dry, sometimes severe |
Dry, persistent and often more severe |
|
Sore throat |
Sometimes |
Common, and often prominent |
|
Runnly or stuff nose |
Sometimes |
Common |
|
Shortness of breath or diffcultly breathing |
Sometimes |
Common, and often prominent |
|
Muscle pain or body aches |
Usual, often severe |
Common |
|
Reapeated shaking with chills |
Rare |
Sometimes |
|
Fatigue |
Early and prominent |
Common |
|
Diarrhea |
Sometimes (more common in children) |
Sometimes (more common in children) |
|
Vomiting or nausea |
Sometimes (more common in children) |
Sometimes (more common in children) |
|
Sudden loss of taste or smell |
Never |
Common |
| Fever |
Temperature of 100°F and above lasting 3-4 days |
Temperature of 100°F and above lasting 2-7 days |
There are some key differences between influenza and COVID-19. COVID-19 seems to spread more easily than flu and cause more serious illness in some people. It may take longer for people to show symptoms, and people may be infected for a longer time. Another important difference is that there is a vaccine to prevent influenza. Currently in the United States, the supply of COVID-19 vaccine is limited, but in the coming weeks and months, the supply will increase. The best way to prevent infection is to avoid exposure to the virus. More
1. Know how it spreads
● COVID-19 spreads easily from person to person, mainly by the following routes:
Between people who are in close contact with one another (within 6 feet).
Through respiratory droplets produced when an infected person coughs, sneezes breathe, sings, or talks.
● Respiratory droplets cause infection when they are inhaled or deposited on mucous membranes, such as those that line the inside of the nose and mouth.
● People who are infected but do not have symptoms can also spread the virus to others.
2. Less common ways COVID-19 can spread
● Under certain circumstances (for example, when people are in enclosed spaces with poor ventilation), COVID-19 can sometimes be spread by airborne transmission.● COVID-19 spreads less commonly through contact with contaminated surfaces.
● Wash your hands often with soap and water for at least 20 seconds especially after you have been in a public place, or after blowing your nose, coughing, or sneezing.
● It' s especially important to wash:
- Before eating or preparing food
- Before touching your face
- After using the restroom
- After leaving a public place
- After blowing your nose, coughing, or sneezing
- After handling your mask
- After changing a diaper
- After caring for someone sick
- After touching animals or pets
● If soap and water are not readily available, use a hand sanitizer that contains at least 60% alcohol. Cover all surfaces of your hands and rub them together until they feel dry.
● Avoid touching your eyes, nose, and mouth with unwashed hands.
4. Avoid close contact
● Inside your home: Avoid close contact with people who are sick.
If possible, maintain 6 feet between the person who is sick and other household members.
● Outside your home: Put 6 feet of distance between yourself and people who don’t live in your household.
- Remember that some people without symptoms may be able to spread the virus.
- Stay at least 6 feet (about 2 arms’ length) from other people.
- Keeping distance from others is especially important for people who are at higher risk of getting very sick.
5. Cover your mouth and nose with a mask when around others
● Masks help prevent you from getting or spreading the virus.
● You could spread COVID-19 to others even if you do not feel sick.
● Everyone should wear a mask in public settings and when around people who don’t live in your household, especially when other social distancing measures are difficult to maintain.
● Masks should not be placed on young children under age 2, anyone who has trouble breathing, or is unconscious, incapacitated, or otherwise unable to remove the mask without assistance.
● Do NOT use a mask meant for a healthcare worker. Currently, surgical masks and N95 respirators are critical supplies that should be reserved for healthcare workers and other first responders.
● Continue to keep about 6 feet between yourself and others. The mask is not a substitute for social distancing.
● Always cover your mouth and nose with a tissue when you cough or sneeze or use the inside of your elbow and do not spit.
● Throw used tissues in the trash.
● Immediately wash your hands with soap and water for at least 20 seconds. If soap and water are not readily available, clean your hands with a hand sanitizer that contains at least 60% alcohol.
7. Clean and disinfect
● Clean AND disinfect frequently touched surfaces daily. This includes tables, doorknobs, light switches, countertops, handles, desks, phones, keyboards, toilets, faucets, and sinks.
● If surfaces are dirty, clean them. Use detergent or soap and water prior to disinfection.
● Then, use a household disinfectant.
8. Monitor Your Health Daily
● Be alert for symptoms. Watch for fever, cough, shortness of breath, or other symptoms of COVID-19.
Especially important if you are running essential errands, going into the office or workplace, and in settings where it may be difficult to keep a physical distance of 6 feet.
● Take your temperature if symptoms develop.
- Don’t take your temperature within 30 minutes of exercising or after taking medications that could lower your temperature, like acetaminophen.
9. Protect Your Health This Flu Season
It’s likely that flu viruses and the virus that causes COVID-19 will both spread this fall and winter. Healthcare systems could be overwhelmed treating both patients with flu and patients with COVID-19. This means getting a flu vaccine during 2020-2021 is more important than ever.
While getting a flu vaccine will not protect against COVID-19 there are many important benefits, such as:
● Flu vaccines have been shown to reduce the risk of flu illness, hospitalization, and death.
● Getting a flu vaccine can also save healthcare resources for the care of patients with COVID-19.

